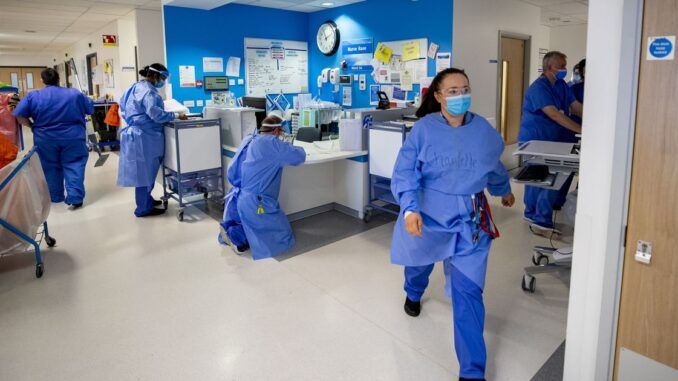
A report by UK MP’s says that England is now short of 12,000 hospital doctors and more than 50,000 nurses and midwives.
They found that high numbers of medical staff are quitting but not being replaced.

BYPASS THE CENSORS
Sign up to get unfiltered news delivered straight to your inbox.
You can unsubscribe any time. By subscribing you agree to our Terms of Use
Warning that this was the worst workforce crisis in NHS history, the report said a reluctance to fill the staffing gap could threaten plans to tackle the Covid treatment backlog.
BBC reports: The government said the workforce is growing and NHS England is drawing up long-term plans to recruit more staff.
Former Health Secretary Jeremy Hunt, who chairs the Commons health and social care select committee that produced the report, said tackling the shortage must be a “top priority” for the new prime minister when they take over in September.
“Persistent understaffing in the NHS poses a serious risk to staff and patient safety, a situation compounded by the absence of a long-term plan by the government to tackle it,” he said.
‘I feel undervalued and taken advantage of’
Simon (not his real name) has worked in the NHS all his career as a psychologist – despite the fact he could have earned more in the private sector.
But next year he will be leaving, moving out of health care altogether, saying the final straw was the below-inflation pay rise this year.
“I now feel totally unvalued and taken advantage of.
“I could have earned twice as much in the private sector, but I stuck with the NHS for my whole career.
“I was pretty convinced I was going, but the latest increase, which isn’t an increase in real terms.
“I can’t blame my employers, their hands are tied by national budgets.
“We truly are in a crisis. We’ve been in economic downturns, but nothing as bad as this.”

The cross-party committee saw evidence that, on current projections, almost a million new jobs will need to be filled in health and social care by the early part of the next decade.
Extra staff would be needed to keep up with rising demand as the population gets older and healthcare becomes more complex and technologically advanced.
The health services in Scotland, Wales and Northern Ireland have faced similar staffing pressures.
A ‘national scandal’
An accompanying report found that rates of harassment and abuse in the NHS were concerningly high with 28% of staff experiencing at least one incident of bullying in the last twelve months.
The committee also heard evidence from former Health Secretary Sajid Javid, who resigned earlier this month, that the government was not on track to deliver its manifesto commitment to increase the number of GPs in England by 6,000.
There was concern about maternity services, with more than 500 midwives leaving the health service between March 2021 and March 2022.
The committee described a situation where NHS pensions arrangements meant some senior doctors were better off retiring or reducing their working hours as a “national scandal” and called for swift action to change the rules.
It said conditions were “regrettably worse” in social care, with 95% of care providers struggling to hire staff and 75% finding it difficult to retain existing workers.
“Without the creation of meaningful professional development structures, and better contracts with improved pay and training, social care will remain a career of limited attraction, even when it is desperately needed,” the report said.
It called for HM Revenue and Customs (HMRC) to be more proactive in enforcing the minimum wage, amid concerns that 17,000 care workers were paid below the legal rate of £9.50 an hour.
Miriam Deakin, deputy chief executive of NHS Providers which represents hospitals, mental health trusts and ambulance services, said that many staff were facing “unsustainable” workloads in the face of “ever-growing demand”.
“The answer is staring everyone in the face: The government must come up with a fully-funded, long-term workforce plan for the NHS,” she said.
Patricia Marquis, England director at the Royal College of Nursing, said the risk to staff and patients from low staffing levels should “shock ministers into action”.
Niamh Harris
Latest posts by Niamh Harris (see all)
- Without Defining ‘Pandemic’ WHO Wants Sweeping Global Power Over Pandemic Policy - April 16, 2024
- Pfizer Is Seeking FDA Approval For RSV Vaccine For Young Adults - April 16, 2024
- Zelensky Pleads With The West To Treat Ukraine Like Israel - April 16, 2024


Stop making everyone sick then .People should be the healthiest in history but it seems they’ve never been so sick and needy ever before. Whose causing that ?