Researchers from Weill Cornell Medical College collected DNA samples at 466 subway stations in New York last summer in an attempt to study the microbiology of urban environments.
They found 15,152 different life-forms invisible to fellow travellers but very much alive in the subway system. While most of the viruses and bacteria found were harmless, others like the bubonic plague they found were not.
Wsj.com reports:

BYPASS THE CENSORS
Sign up to get unfiltered news delivered straight to your inbox.
You can unsubscribe any time. By subscribing you agree to our Terms of Use
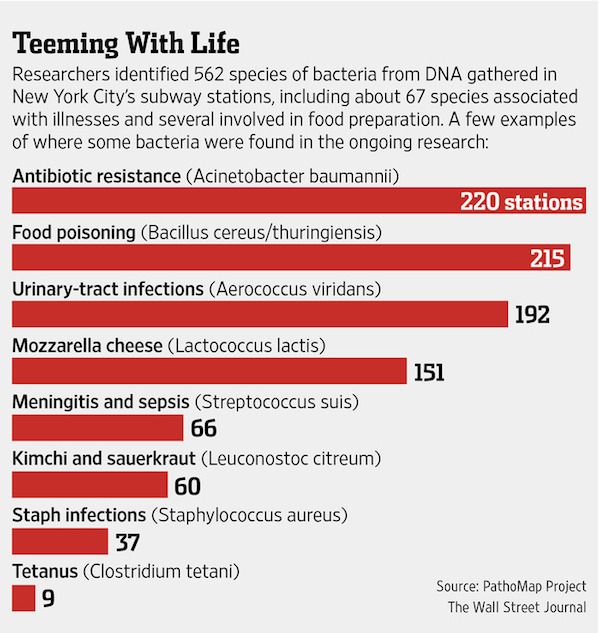
In 18 months of scouring the entire system, he has found germs that can cause bubonic plague uptown, meningitis in midtown, stomach trouble in the financial district and antibiotic-resistant infections throughout the boroughs.
Frequently, he and his team also found bacteria that keep the city livable, by sopping up hazardous chemicals or digesting toxic waste. They could even track the trail of bacteria created by the city’s taste for pizza—identifying microbes associated with cheese and sausage at scores of subway stops.
The big-data project, the first genetic profile of a metropolitan transit system, is in many ways “a mirror of the people themselves who ride the subway,” said Dr. Mason, a geneticist at the Weill Cornell Medical College.
It is also a revealing glimpse into the future of public health.
Across the country, researchers are combining microbiology, genomics and population genetics on a massive scale to identify the micro-organisms in the buildings and confined spaces of entire cities.
By documenting the miniature wildlife, microbiologists hope to discover new ways to track disease outbreaks—including contagious diseases like Ebola or measles—detect bioterrorism attacks and combat the growing antibiotic resistance among microbes, which causes about 1.7 million hospital infections every year.
“We know next to nothing about the ecology of urban environments,” said evolutionary biologist Jonathan Eisen at the University of California at Davis. “How will we know if there is something abnormal if we don’t know what normal is?”
Dr. Mason and his research team gathered DNA from turnstiles, ticket kiosks, railings and benches in a transit system shared by 5.5 million riders every day. They sequenced the genetic material they found at the subway’s 466 open stations—more than 10 billion fragments of biochemical code—and sorted it by supercomputer. They compared the results to genetic databases of known bacteria, viruses and other life-forms to identify these all-but-invisible fellow travelers.
In the process, they uncovered how commuters seed the city subways every day with bacteria from the food they eat, the pets or plants they keep, and their shoes, trash, sneezes and unwashed hands. The team detected signs of 15,152 types of life-forms. Almost half of the DNA belonged to bacteria—most of them harmless; the scientists said the levels of bacteria they detected pose no public-health problem.
As more and more scientists probe urban microbiology, they are also hoping to find ways to foster beneficial bacteria through building design and to learn how to eliminate construction practices that create living conditions for the germs that make people ill.
This emerging field reflects the growing awareness that the human body swarms with bacteria. Typically, every person is home to about a hundred trillion microbial cells bearing five million different genes, totaling about 5 pounds of micro-organisms per person. Indeed, microbes in and on the body outnumber human cells about 10 to one.
“You are a minority party in the democracy of the body,” Dr. Mason said.
The body’s collection of microbes, called the microbiome, influences health in ways that researchers are only beginning to understand. They may be key to proper digestion, vitamin synthesis and brain function, new research suggests. Changes among the millions of microbes living in the human stomach also may promote obesity, trigger ulcers or affect how well a flu vaccine works.
Broadly speaking, city living leaves its mark on people. That includes the sorts of microbes that collect inside them. A recent comparison of urban and rural residents in Russia found that city dwellers had different sets of stomach microbes than people in the countryside.